Slipped Disc
Slipped Disc
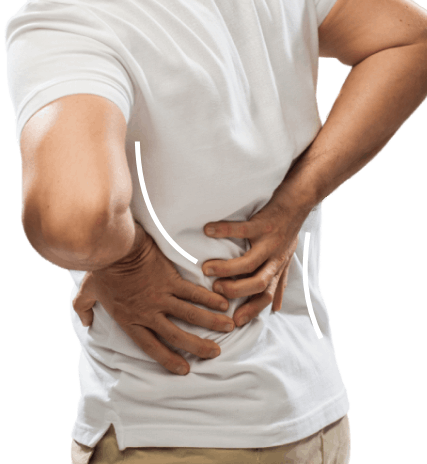
Many may not be aware that they have a slipped disc or herniated disc because it can be dismissed as a muscle strain or pain. However, the latter usually goes away within six weeks, and pain caused by a slipped disc worsens over time. Another telltale sign that it could be more than just a strain is when one experiences numbness or pain radiating down the legs, because nerves that run from the spine to the foot have been pinched. Unfortunately, a patient can only confirm the diagnosis after a magnetic resonance imaging (MRI) is done.
It can be easy to ignore the discomfort caused by a slipped disc when the condition is mild, as it might not be very severe and some do not experience radiating pain down the legs. Some may even suffer for years before approaching medical help! However, the risk of leaving it untreated is that it might lead to complications, such as incontinence because the disc adds pressure to the nerves affecting the bladder or bowel. In some cases, partial paralysis might even result when the disc pushes or presses against the nerve leading to the lower limbs.
Understanding Spinal Disc
A spinal column consists of a series of bones stacked onto each other, also known as your vertebrae. This column includes seven bones in the cervical spine, 12 in the thoracic spine and five in the lumbar spine, ending with the sacrum and the coccyx. Discs cushion the bones and protect them from shocks that we incur through walking, lifting and jumping.
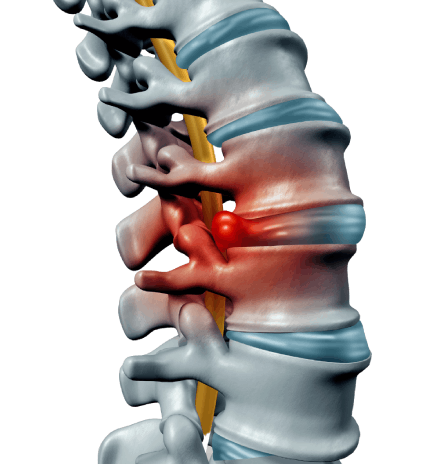
Each disc comprises of a semi-solid, gelatinous inner compartment (nucleus pulposus) and a hard outer (annular) ring. Injury or weakness (such as annular tear) may cause the inner part to protrude through the external ring, and that’s when a slipped, herniated or prolapsed disc occurs. This process causes pain and discomfort. If the slipped disc compresses a spinal nerve, you may experience numbness or pain in the neck, back or arms and/or legs. In very severe cases, the nucleus pulposus may detach from the disc entirely, occupy the space in the spinal canal and cause severe nerve compression, resulting in nerve injury (such as myelopathy).
Causes of Slipped Disc
When the outer annular ring becomes weak or torn, the nucleus pulposus may slip out. This can be due to age or trauma from to certain motions such as twisting or turning when lifting an object. Heavy or large objects place immense strain on the lower back, possibly resulting in slipped discs. Therefore, those whose jobs require a lot of lifting are at risk. People who are overweight are also at risk because the discs need to support the body weight. Individuals who have weak muscles or lead sedentary lifestyles are prone to develop slipped discs.
As you age, your discs begin to degenerate and lose their protective water content and that means that its easier for the inner compartment to slip out of place. Discs may also lose their elasticity due to wear and tear. Activities that put pressure on the spine will contribute to wear and tear of discs. Even poor posture or incorrect exercise routines (e.g.weight lifting in a gym workout) can put unnecessary pressure on the back.
Risk Factors
If you display the following risk factors, you may be more predisposed to developing the condition, although it can also occur regardless of age or health condition:
- Ageing and degeneration – When one ages, the risk of experiencing a slipped disc increases as our discs may lose their elasticity and become more prone to damage.
- Woman at perimenopausal age
- Men are twice as likely to develop a herniated disc compared to women
- Occupation: People with physically demanding jobs have a greater risk of back problems. – Repetitive lifting, pulling, pushing, bending sideways and twisting also can increase your risk of a herniated disk.
- Genetics – Those with a family history have a higher chance of developing one.
- Smoking – One lesser-known cause of slipped discs is smoking. Cigarettes and other tobacco products contain toxins that prevent your discs from getting the nutrients they need to stay healthy and flexible. This contributes to the acceleration of disc degeneration or disc damage.
Symptoms of Slipped Disc
The herniated disc can be anywhere along the back on even in the neck, so symptoms depends on where it is situated, and whether a nerve is compressed. The discomfort usually occurs on one side of the body, although it can present as central or both sides of the body.
- Pain in the arm or leg
If the slipped disc is in the lower back, the pain will be in your back, buttocks, thighs, calves and ankles. It will radiate all the way down to the foot, especially with prolong walking or standing. If the slipped disc is in the neck, the pain is felt in the neck, shoulders, arms or fingers. Coughing and sneezing may cause a sudden pain to shoot through your limbs. The pain is commonly described as a sharp or burning sensation, similar to an electric shock. Activities such as lifting, bending, sitting or twisting may increase the pain, while lying down will provide relief. In some instances, pain can be aggravated by lying down, causing radiating pain and numbness of hands and legs, affecting sleep. - Numbness or tingling sensations
When the disc presses down on a nerves, you may feel numbness or tingling radiating down the affected areas, usually down the leg. You may also experience cramping or muscle spasms, including weakness and loss of strength. - Weakness
Compressed nerves tend to weaken the surrounding muscles. When weakness sets in, it is a sign that the slipped disc condition is serious. The nerve compression is severe enough to cause nerve injury, resulting in loss of strength. Weakened muscles can cause instability in movement, resulting in stumbling or ability to lift or hold items. Weakness can manifest when foot drops occur (your foot flops when you walk) or inability to climb stairs. In severe cases, there can be loss of bowel or bladder control. - Pain may develop quickly and leave within six weeks
The pain usually comes on fast, and you might not be able to associate a specific injury or traumatic event for the cause. The symptoms however, don’t last too long. Nearly 70% of people who experience painful lumbar disc herniation may report within 6 weeks that they no longer feel the pain, even if they received no medical treatment for it. If you experience back pain or leg pain that occurs for a few days and then disappears, that may suggest a mild herniated disc, without nerve impingement.
Take-home Message
Not all slipped disc conditions needs surgical intervention. Only when there is nerve impingement and compression, then treatment will be needed to target at freeing the trapped nerve. Conversely, in other non-compressive cases, surgery is to stop pain and get rid of the pain generator. This procedure, however, does not reverse the degeneration nor wear and tear of the damaged disc.
Once a slipped disc, it always will stay an injured disc. Pain may even improve spontaneously if there is minimal mechanical compression on the spinal nerves. After the back or neck pain has been resolved, there is still a risk of further degeneration and worsening of the condition in future.
Discs can get herniated without showing signs or symptoms. In such cases, the condition can only be diagnosed through scans such as MRIs.
Diagnosing Slipped Disc
Doctors will initially perform a physical exam by checking the area of pain and discomfort. They will test your strength and nerve function by getting you to perform certain movements and will then touch your affected area to evaluate the sensitivity to match your pain to the respective affected spinal segment. You should also tell your doctor what activities or movements tend to aggravate the pain. Sharing your medical history will also give your doctor a clearer picture of the condition.
Imaging tests are often necessary in diagnosing the problem. The scans include X-rays, CT scans, MRIs and discograms. With these information, your doctor is able to tell you if what you are experiencing is due to a herniated disc.
When To See Doctor?
Waiting too long to seek medical help may lead to serious complications. A study was conducted in 2011, comparing two groups of patients. The group that waited longer than six months to report their herniated disc symptoms to a doctor did not respond as well to treatment as those who waited less than six months to seek medical advice. You shouldn’t wait too long to before visiting the doctor, especially if your pain is severe. Over time, the slipped disc may cause long-term nerve damage and injury, that is unlikely to respond to treatment at all subsequently.
Sinister Signs and Symptoms
If you experience any of the following symptoms, you should contact your doctor immediately:
- Loss of bowel and/or bladder control, loss of feeling in your lower legs and feet or upper limbs and hands/fingers. These may be signs of cauda equina syndrome, a rare but serious spinal disorder.
- Loss of balance and fine motor skills and muscle weakness. These are signs of signal spinal nerve compression. The herniated disc can even compress the spinal cord itself, resulting in a condition named myelopathy
- Persistent pain lasting more than 3 months. Even after several weeks of conservative treatment, such as with ice, heat or stretching, your symptoms don’t respond or worsen
- Pain affecting daily function and sleep. Your pain is debilitating and getting in the way of your day-to-day activities (causing you to miss work or social events). If your sleep is interrupted and affected by pain, causing sleep deprivation and low energy.
The sooner you consult medical help, the higher the chances of early treatment that will lead to complete recovery. It is not recommended to wait for the symptoms to disappear as irreparable nerve damage may occur.
Treatment Options
General Slipped Disc Treatment
Nevertheless, during a period of recovery, avoid bending, lifting and prolonged sitting. If you experience severe back pain, rest in bed for one or two days on a firm surface or mattress. You can slowly introduce light physical activity thereafter to keep your spine flexible. Hence, for the best treatment for slip disc, the key factor is that you should not wait too long to seek proper treatment.
Treatments by Doctors
The target of exercise is to build tolerance and back conditioning. Slipped disc pain is not a muscle injury pain whereby you should work through or engage the pain. While exercising, you should pace yourself progressively, be pain contingent but not ignore the pain signal warnings during workout.
If normal painkillers do not work, your doctor may prescribe stronger medication such as narcotics or nerve pain medication.
In very severe cases, one out of ten sufferers require surgery. This is the final option and only suggested after all the conservative methods have been exhausted. Your surgeon may remove the damaged or protruding portion of the disc without removing the entire disc. This is called a microdiscectomy. You doctor may have to replace the disc with an artificial one or remove the disc and fuse your vertebrae together in extreme cases. This procedure is coupled with laminectomy and spinal fusion to add stability to your spinal column. Surgery solves the mechanical nerve compression caused by the slipped disc, and the pain will be relieved immediately but physiotherapy is then required to rehabilitate the patient’s back muscles.
Minimally Invasive Procedures/ Injection
Prevention
There are ways to prevent a slipped disc from occurring, and these prevention points are good to follow especially if you are at risk of having a herniated disc.
- Maintain a healthy weight
- Exercise moderately and regularly (e.g. brisk walking and swimming)
- Maintain a good posture when sitting or standing
- Lift heavy objects the right way (by using your legs, not your back, bend your knees, squat and lift)
Get Your Pain Resolved
Send your enquiries or consult our pain experts today.


