Spinal Stenosis
Spinal Stenosis
Spinal stenosis (or narrowing) is a common condition that occurs when the small spinal canal that contains the nerve roots and spinal cord becomes restricted. This narrowing can squeeze the nerves and the spinal cord, causing lower back and leg pain. In general, spinal narrowing is caused by crowding within a limited space, such as thickened tissue or bone growing into the canal or a surrounding disc has protruded, resulting in narrowing of the canal space.
This results in a “pinching” of the spinal cord and/or nerve roots. Typically, a person with spinal stenosis will complain about developing deep ache and intense pain in the legs or calves and lower back after walking. Pain comes on more quickly when walking uphill. This is usually very reproducible and immediately relieved by sitting down or leaning over. When the spine is bent forward, more space is available for the spinal cord, causing a reduction in symptoms.
Although symptoms may arise from narrowing of the spinal canal, not all patients with such narrowing develop symptoms. It remains unknown why some patients develop symptomatic stenosis and others do not.

Causes of Spinal Stenosis
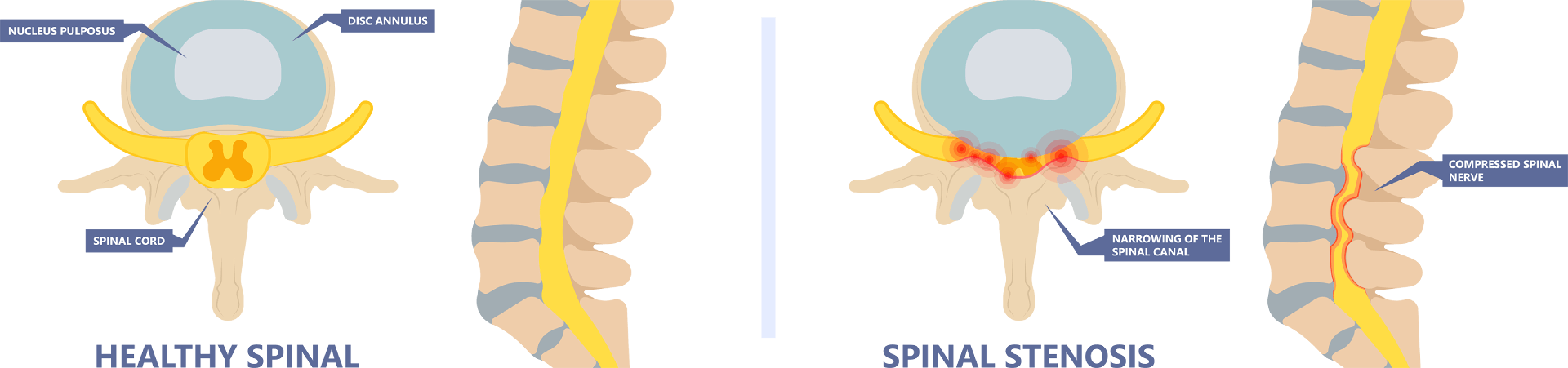
Unless the individual is born with a small spinal canal (congenital stenosis), spinal narrowing most commonly results from progressive degenerative changes. This acquired spinal stenosis can occur from the narrowing of the space around the spinal cord due to bony overgrowth from osteoarthritis combined with thickening of one of the ligaments in the back, and a bulge of the intervertebral discs. The risk of developing spinal stenosis increases in those who:
- Are born with a narrow spinal canal
- Are female
- Are 50 years of age or older
- Are overweight with BMI more than 30
- Have had previous injury or surgery of the spine
- Have poor posture
Symptoms of Spinal Stenosis
Your symptoms may include:
- Numbness
- Weakness
- Cramping
- Pain in the legs and thighs
- Radiating pain down the leg
- Abnormal bowel and/or bladder function
- Decreased sensation in the feet causing difficulty placing the feet when walking
- Loss of sexual function
- Partial or complete leg paralysis
The pain experienced from spinal stenosis varies, depending upon the site of compression. If the upper spinal cord is involved, it can cause midline neck/back pain. If compression progresses, it may lead to myelopathy (compression of the spinal cord) or cauda equina syndrome (compression of the distal tail of the cord). Symptoms include a drastic change in walking pattern, upper extremity spasms, lower extremity weakness, and bowel and bladder incontinence. When the site of entrapment is the intervertebral foramen, the arms and/or legs may be involved. There may be pain, numbness/tingling, cramping and/or weakness in the involved limb. The spectrum of symptoms is from mild to severe, the latter requiring urgent attention (refer to low back pain).
Diagnosing Spinal Stenosis
Your doctor will ask about your symptoms and medical history, and perform a physical exam, including specialized manoeuvres that will detect whether the pain is worsened by making the spinal canal smaller, or improved by making the canal larger. Additional tests conducted to confirm and assess the diagnosis may include X-ray of the spine, CT scan, MRI scan, etc.
Treatment Options
Although there is no spontaneous recovery for spinal stenosis, various therapies are available, one of the most important being exercise. Your doctor will determine whether you are appropriate for conservative treatment versus surgical treatment. Most cases of spinal stenosis can be treated with the following:
- Anti-inflammatory medications as well as nerve stabilising medications.
- Strengthening programs and modalities in physical therapy, including soft laser therapy.
- Interventional procedures, such as laser ballooning injections to free the nerves (refer to Neuroplasty)
- Open surgical decompression by removal of the skeletal bone.
Get Your Pain Resolved
Send your enquiries or consult our pain experts today.


